GLP-1: Should I, or Shouldn’t I? Understanding What It Really Does to the Body
In recent years, GLP-1 medications have quickly become one of the most talked-about tools for weight loss. As their popularity has grown, I have been asked several times what I think about these medications.
When the question first came up, I chose not to give an immediate opinion. As a Functional Nutrition Counselor, I believe it is important to research and understand how something works in the body before speaking about it publicly. This is a longer blog but stay with me through to the end where I’ll summarize the key points and share my perspective.
My hesitation to promote this medication also comes from personal experience of utilizing a lot of medications to tackle my health issues. After years of taking medications for issues such as sinus infections and gut problems and later learning how repeated antibiotic use can disrupt the gut microbiome, I became much more cautious about anything that alters the body’s natural systems from a medication perspective. Food can also alter how the body functions, but that is a topic we will explore in another post.
Medications certainly have an important place in medicine and can be lifesaving in times of crisis. However, when medications are used as long-term solutions, it raises important questions about what is happening inside the body and why those symptoms developed in the first place.
Before evaluating GLP-1 medications, it helps to first understand how the body naturally produces and uses GLP-1 to regulate blood sugar, appetite, and energy. From there, we can better understand how these medications interact with that system and why they lead to weight loss.
Another important consideration is what happens when the medication is stopped. If underlying eating habits and lifestyle patterns are not addressed, many individuals find the weight returns once the medication is discontinued. This raises important questions about whether GLP-1 medications should be viewed as a long-term management tool or a temporary aid while deeper lifestyle changes are developed. We also need to consider the potential effects to the body when remaining on these medications long-term.
Let’s dive in!
WHAT IS GLP-1?
GLP-1 stands for Glucagon-Like Peptide-1. This is a hormone produced in the intestines and released after we eat. Its role is to help the body regulate blood sugar and appetite by signaling the pancreas to release insulin.
HOW DOES GLP-1 WORK?
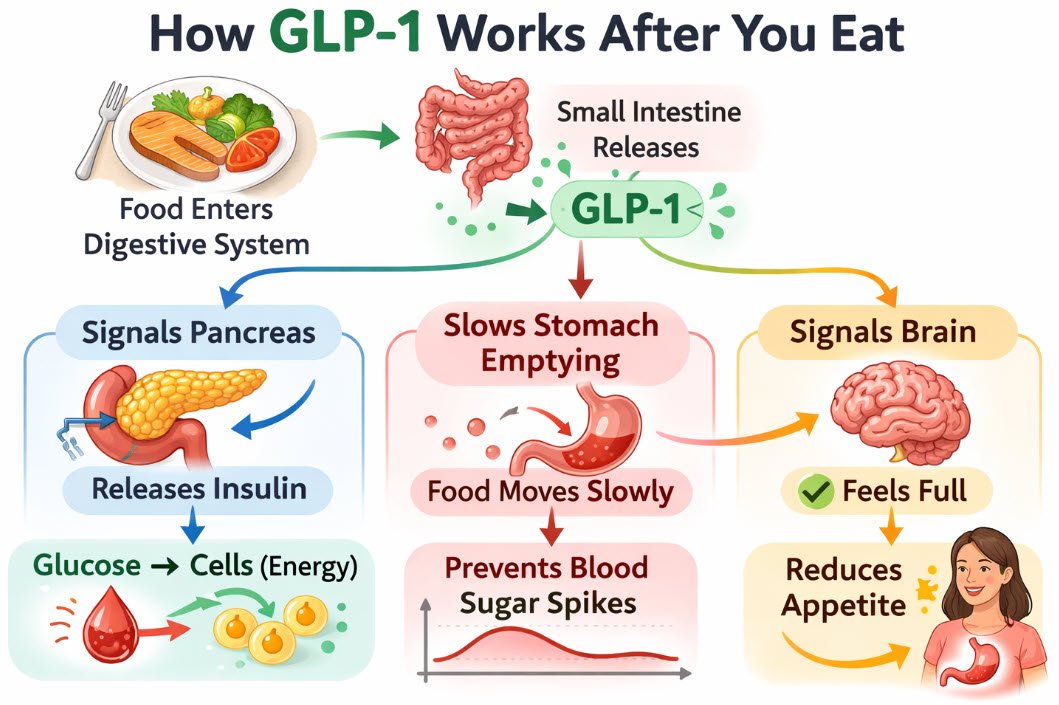
Now that we have a brief understanding of what GLP-1 is and its role, let’s look at how this process works inside our bodies after food enters the digestive system. There are several processes that begin working together and they are as follows:
The intestines release GLP-1.
First, specialized cells called L-cells in the small intestine release the hormone GLP-1 in response to nutrients from food. L-cells job in the body is to sense nutrients from food and release hormones that help regulate digestion and blood sugar.
GLP-1 signals the pancreas.
Second, this hormone sends a signal to the pancreas telling it to release insulin. Insulin helps move glucose (sugar) from the bloodstream into the cells where it can be used for energy.
GLP-1 slows stomach emptying.
Third, this helps food move through the digestive system more slowly, which prevents rapid spikes in blood sugar.
GLP-1 communications with the brain.
Fourth, signals are sent to the brain that contribute to feelings of fullness and satisfaction after eating.
I often find that visuals help make complex processes in the body easier to understand. Below is a simple illustration that shows how these steps work together within the body.
Image credit: Created with ChatGPT (OpenAI)
WHY INTERVENTION HAPPENS?
In conventional medicine, GLP-1 drugs are considered an intervention for:
Type 2 diabetes
Obesity
Metabolic Syndrome
Genetics and metabolic predisposition
Highly processed diets
Chronic stress and cortisol imbalance
Sedentary lifestyle
Poor sleep
Insulin resistance
Disrupted hunger and fullness signals
So GLP-1 is used to help regulate blood sugar, reduce appetite, and assist with weight loss when other methods have not been successful.
From a functional lens, or root cause perspective, this medication would be viewed as a management strategy rather than a root-cause solution. Instead, we need to address underlying contributors such as:
Poor metabolic flexibility (the body’s reduced ability to switch between burning carbs and fat for energy)
Ultra-processed diets
Gut dysfunction
Insulin resistance
Chronic stress and cortisol dysregulation
Sleep deprivation
Sedentary lifestyle
Genetics
Environment
IMPACT OF LONG-TERM USE
In my research, I looked for all of the impacts of long-term use of this medication. There are several, and I know your medical practitioner will share them with you, but here are the top three:
Gastrointestinal Problems - GLP-1 slows down stomach emptying which can cause nausea, vomiting, constipation, diarrhea, and stomach discomfort.
Loss of Lean Muscle Mass - A portion of the weight lost comes from lean muscle mass, not just fat. Muscle supports metabolism, stabilizes blood sugar, and protects bone density, especially for women in midlife and post-menopause. A loss of muscle mass is known as sarcopenia. As we age, maintaining muscle becomes increasingly important because it supports strength, stability, metabolic health, and overall function of the body.
Weight Regain After Stopping - Studies show that many people regain a significant portion of the weight once the medication is discontinued. When appetite suppression is stopped, our normal hunger signals return, and if lifestyle habits haven’t changed, weight regain is common.
There are many more side-effects and I encourage everyone to research this prior to making a decision before going on GLP-1 and of course discuss it in detail with your medical practitioner to help you make the right decision.
SUMMARY
If asked the question again, this is how I would respond. If all other avenues have been explored and the root causes of what is occurring inside the body are still being investigated, GLP-1 medications could be used as a short-term tool to help initiate progress. At the same time, attention should be placed on improving lifestyle patterns and developing a deeper understanding of digestive health, because many aspects of metabolic regulation begin in the gut.
Since my primary focus is helping individuals address digestive imbalances, it is important to consider how medications like GLP-1 may further impact those systems. As part of my training in functional nutrition, I approach topics like this by looking at the broader systems involved in metabolic health. In my view, three key areas influence how the body regulates weight and metabolism: digestion, genetics, and inflammation. Outside of genetic factors, weight gain is often influenced by digestive dysfunction and chronic inflammation. For this reason, my approach centers on understanding what is happening within the digestive system and working to restore balance at that level.
Another factor that is often overlooked is socioeconomic influence. Access to healthy foods, nutrition education, financial resources, and time for meal preparation can significantly impact dietary habits and long-term metabolic health. These environmental factors can contribute to the conditions that eventually lead some individuals to seek medical interventions such as GLP-1 medications.
I would also recommend engaging a functional nutrition counselor to work alongside your medical practitioner to help guide lifestyle changes and provide education on how food and digestion influence metabolic health. I would also encourage attending educational talks or workshops that help you better understand your body and how it functions. The more you learn, the more empowered you become to make lifestyle choices that support optimal health.
I encourage everyone to do their own research when considering medications and to bring their questions to their medical practitioners so they can make informed decisions. Ultimately, the goal is to determine the best course of action for you as the individual and what supports your long-term health.
References:
Holst JJ. The physiology of glucagon-like peptide 1. Physiol Rev. 2007 Oct;87(4):1409-39. doi: 10.1152/physrev.00034.2006. PMID: 17928588.
Drucker DJ. Mechanisms of Action and Therapeutic Application of Glucagon-like Peptide-1. Cell Metab. 2018 Apr 3;27(4):740-756. doi: 10.1016/j.cmet.2018.03.001. PMID: 29617641.
Shah M, Vella A. Effects of GLP-1 on appetite and weight. Rev Endocr Metab Disord. 2014 Sep;15(3):181-7. doi: 10.1007/s11154-014-9289-5. PMID: 24811133; PMCID: PMC4119845
Author Note:
This article was developed using a combination of published research, professional training in functional nutrition, and AI-assisted writing tools to help organize and communicate the information clearly.